Header start
- Home
- Keio Times Index
- Keio Times
Content start
"Keio Donner Project" Accelerating
COVID-19 Research
Aug. 4, 2020
The Birth of "Keio Donner Project"
for COVID-19 with its Original Core Values
Prompted by their concern for the similar crisis and desire to help, research projects started to be built under the leadership of the top officials of Keio University, Tsutomu Takeuchi (Rheumatology, Vice-President), Masayuki Amagai (Dermatology, Dean of the School of Medicine), and Yuko Kitagawa (Surgery, Hospital Director General). The purpose of the research projects was to clarify the mechanism of COVID-19 disease, increase diagnostic test capacity, and develop effective therapeutic options.
Recognizing its original core values, Keio University held its first COVID-19 strategic meeting on April 2nd, where clinical and basic scientists discussed how to deliver their expertise and strengths to meet the current needs of the society. Projects on developing neutralizing antibody detection system and convalescent plasma therapy were launched from the initial meeting, and as it unfolded, other projects developed, such as the epidemiological project and the SARS-CoV-2 viral genome sequencing project. The COVID-19 research team now consists of more than 150 people, and a Web Meeting has been held on a weekly basis, with updates and progress being reported from each project. The aforementioned projects were collectively named as "Keio Donner Project" by our dean, Dr. Masayuki Amagai.
"Keio Donner Projects" was set out to face the outbreak of COVID-19, and aims to 1) remind ourselves of how and where Keio University Hospital started with our founder Sibasaburo Kitasato, 2) accelerate the research on infection, immunity, and inflammation, and 3) to nurture human resources. Our current approaches to develop neutralizing antibodies and convalescent plasma therapy root back to Dr. Kitasato, who discovered and established the diphtheria antitoxin serum therapy. At that time, medical students learned the German language. Dr. Kitasato was called "Donner sensei" by his students who had a feeling of awe and respect for him. The word "der Donner" in German means thunder. Returning to the starting point has stimulated scientists at Keio to work as one team to unravel the new coronavirus disease. Here are some of the active projects.
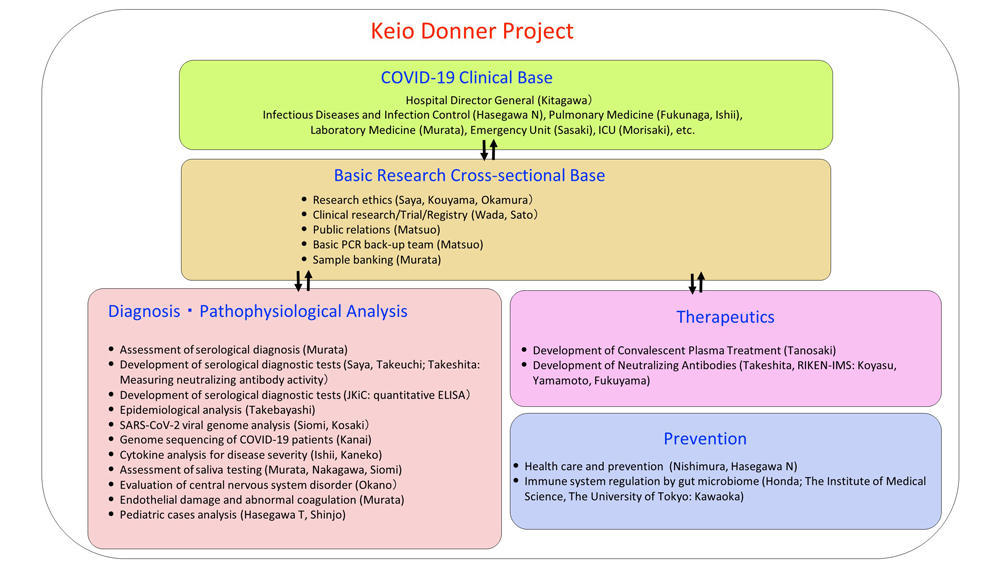
Qualitative and Quantitative Assays
of Anti-SARS-CoV-2 Antibody
A joint research team led by Dr. Mitsuru Murata (Laboratory Medicine) and Dr. Hideyuki Saya (Institute for Advanced Medical Research) has begun to test several commercially available antibody assay kits. Serum samples obtained from COVID-19-suspected patients who have undergone PCR analysis will be tested with these kits, to determine the proper timing of detection and to evaluate the sensitivity and specificity of each assay. Moreover, another joint group in this team, led by Dr. Tsutomu Takeuchi (Division of Rheumatology, Internal Medicine) is developing an original method for detecting anti-SARS-CoV-2 neutralizing antibodies.
Viral Genome Sequencing of SARS-CoV-2
from Keio Samples
To track the evolution and spread of SARS-CoV-2 over time, comparing viral genome sequencing data and identifying mutation patterns are important. Nextstrain (Nextstrain.org) is an open-source application to analyze viral genome data shared by researchers from all over the world via GISAID (Global Initiative on Sharing All Influenza Data) and provides visualization of the evolution of SARS-CoV-2.
Our research team led by Drs. Haruhiko Siomi (Molecular Biology) and Kenjiro Kosaki (Medical Genetics) has started sequencing the viral genomes derived from COVID-19 patients at Keio University Hospital. By analyzing the viral genome sequences, they hope to accurately trace the source of the virus. For example, in the setting of nosocomial infections or when a cluster occurs, we may be able to prevent the further spreading of the virus if we can determine whether it started from one single case, or from several different routes.
Development of Convalescent Plasma Treatment for COVID-19
The potential utility of convalescent plasma to treat COVID-19 is gaining worldwide attention as the U.S. Food and Drug Administration (FDA) has granted approval to start investigational studies using blood plasma collected from individuals who have recovered from COVID-19. Keio University has also initiated a research project led by Dr. Ryuji Tanosaki (Center for Transfusion Medicine and Cell Therapy), in order to develop COVID-19 convalescent plasma treatment. In the first step, medical staff who has recovered from COVID-19 will be recruited as blood donor candidates. These candidates will have to meet the eligibility criteria to become COVID-19 plasma donors, i.e. have fully recovered from COVID-19 for at least two weeks, have consecutively twice tested negative by PCR test, and have a high titer of neutralizing antibody. The collection procedure will be done according to the protocol established by the Japanese Red Cross Society. The rest of the samples will also be allocated to other COVID-19-related research projects. At present, the team is planning to enroll 30 to 50 recovered cases from medical staff at Keio University and Eiju General Hospital.
COVID-19 Epidemiological Project Started
Much is still unknown about the clinical course of COVID-19. There have been reports of various incubation periods or patients getting re-infected after recovery. To capture the severity and magnitude of a pandemic and its transmission routes, monitoring and recording the clinical course of both infected and healthy individuals is critical. COVID-19 epidemiological team (Preventive Medicine and Public Health, Center for Infectious Diseases and Infection Control, Laboratory Medicine, and University Health Center) has started surveillance of the individuals who were tested for SARS-CoV-2 infection by RT-PCR and employees at Keio University Hospital. The output results may boost the effective control of hospital infections. The team is also creating a comprehensive database to link clinical data to viral genome sequence and antibody test results, aiming to identify and prevent nosocomial infections, estimate community infection rate and Infection Fatality Rate (IFR) by screening patients for planned care.
Finding Genetic Factors Associated with Disease Exacerbation by Comprehensive Genomic Analysis on Japanese COVID-19 Patients
Unlike many western countries, mortality rate from COVID-19 is much lower in Japan. Yet, a proportion of patients have their symptoms worsening to death. In order to identify association between genetic factors and disease progression among Japanese COVID-19 patients, "2020 COVID-19 Taskforce" project has been launched. Scientists from various research fields have gathered in this project, including Dr. Takanori Kanai (Gastroenterology and Hepatology, Research Director), Dr. Yuko Kitagawa (Surgery, Hospital Director General), Dr. Koichi Fukunaga (Pulmonary Medicine), Dr. Toshiro Sato (Organoid medicine), and Dr. Naoki Hasegawa (Infectious diseases) from Keio University Hospital. Blood samples derived from around 500-600 COVID-19 patients will be comprehensively analyzed using technologies such as ultra-high-resolution HLA analysis, SNP array analysis, whole genome sequencing, and T-cell repertoire analysis; and by comparing the results of severely ill patients with mild or asymptomatic patients they hope to elucidate important factors which may contribute to the disease progression. They also aim to develop a nasal spray type mucosal vaccine based on their original molecular needle technology (developed at Kitasato University).
Future Prospects of Donner Project
Within a month since the launching of Keio Donner Project, driven by the genuine passion, motivation, and dedication, our team members have created a huge movement to tackle this unprecedented crisis.
Basic researchers and staff at Keio University, who are not usually involved in the daily clinical practice have set up a "Basic Researchers Back-Up Team," to help the projects and more than 100 volunteers have signed up. Other new projects are being initiated, such as basic researchers' PCR back-up team, a task force team to support and enhance clinical trials, a team for host genome analysis, and a public relation (PR) team to provide the latest news and updates on Donner Project. We will continue to work hard together to deliver encouraging news, and we kindly appreciate your continued support.
(Keio Donner Project PR team)



*All affiliations and titles are those at the time of publishing.
Footer start
Navigation start


